How Breast Radiologists Collaborate to Deliver Better Care
When a woman comes in for a routine mammogram, it’s often just one appointment on her calendar: a 20-minute stop before work or after dropping off the kids. But behind that one screening are layers of teamwork, training, and coordinated care, all quietly unfolding in the background.
Breast health is never a solo effort. It’s the product of multiple medical professionals, each bringing their own expertise to the table, and each relying on one another to do their best work.
As a radiology provider, we see this collaboration up close every day. And while the breast radiologist isn’t the one performing surgery or prescribing treatment, she plays a pivotal role in helping those things happen safely, confidently, and at the right time.
It All Starts with the Image
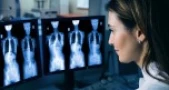
For many patients, a breast radiologist is the first to see something others can’t. While a mammogram might look like a black-and-white puzzle to most of us, radiologists are trained to pick up on subtle distortions, architectural changes, or tiny clusters of calcifications that may be early signs of something more serious.
If a finding raises concern, the radiologist guides the next steps, whether that means a follow-up ultrasound, a diagnostic mammogram with special views, or a breast MRI for more detailed imaging. If needed, the radiologist also performs the biopsy herself, using imaging to precisely sample the tissue in question. That small intervention — usually done in less than an hour — can clarify what’s happening and direct the rest of the care plan.
But the work doesn’t stop with a diagnosis. It’s only just beginning.
Trust Through Teamwork
Once a diagnosis is confirmed, whether it’s cancer, a benign mass, or a high-risk lesion, the patient is typically referred to a breast surgeon. At this point, the radiologist shares detailed imaging and biopsy results to help the surgeon understand the full picture: where the lesion is located, how large it is, and whether there are any other areas of concern in the breast.
Often, the surgeon will ask the radiologist to place a marker — such as a thin wire or a seed — into the lesion before surgery. This helps the surgeon locate it precisely during the operation, even if it’s not visible or palpable. In some cases, radiologists will also be asked to review intraoperative images to confirm that the targeted tissue was successfully removed.
The handoff between radiologist and surgeon is one of trust. One depends on the other to do their job well. That relationship is especially important when the findings are subtle, or when a patient’s anatomy makes imaging more complex, like dense breast tissue or cases involving multiple lesions.
Seeing the Whole Picture
Beyond surgery, radiologists also collaborate with pathologists, who examine the biopsied or surgically removed tissue under a microscope. While pathology provides the cellular-level diagnosis, radiologists bring the full structural and imaging context. Together, they ensure that imaging findings and pathology results line up in a process called radiologic-pathologic correlation. If something doesn’t match, they may flag it for additional review, helping to avoid misdiagnosis or unnecessary treatment.
Radiologists also work closely with medical oncologists, especially when patients undergo chemotherapy or hormone therapy. Through follow-up imaging, the radiologist helps assess how a tumor is responding to treatment, whether new areas of concern have appeared, or whether further biopsies are needed.
Later in the process, radiation oncologists may ask radiologists for help identifying where to target post-surgical radiation. They rely on imaging to visualize the original tumor bed, trace any changes since surgery, and guide treatment in a way that protects healthy tissue while ensuring the cancer is fully addressed.
A Quiet but Essential Role
Patients often meet their surgeon. They talk with their oncologist. They see nurses, navigators, and techs along the way. But they rarely meet the radiologist who first raised the flag, who helped guide the biopsy, and who quietly supported every clinical decision along the way.
At our practice, we think it’s important to help patients understand just how many professionals are working on their behalf. The breast radiologist doesn’t lead the care team, but she plays a consulting, collaborative role that strengthens every link in the chain.
The more closely we work with surgeons, oncologists, and pathologists, the more confident and coordinated our care becomes. And when care is this well-connected, patients benefit from faster answers, clearer decisions, and better outcomes.